Patient decision aids (PtDA) are unbiased information structured to support patients to make informed choices about medical options. We use them to supplement and extend the clinical discussion.
We believe that excellent care begins with an attitude of mutual respect between the physician and patient and expresses itself in open communication where facts, personal values and choice are shared. We have developed PtDA in several formats and used them with thousands of patients with rheumatic diseases over nearly 20 years.
All our patient decision aids aim to present medications in a clear, accurate, and balanced way. They walk the reader through a decision, so they know more about facts and pause to think about what matters most. Though a patient can use them as a self-learning resource, they are designed to complement a face-to-face or virtual doctor patient discussion. The use of PtDA is an important strategy to encourage shared decision making.
One approach is to start with an Option Table Decision Aid , which is appropriate for your decision, and use this to consider all the medication choices. This should enable the team (clinician and patient) to narrow the choices to 1 – 3 medications. Now decision-makers focus and dig deeper by reviewing one or more of our drug specific Patient Decision Aids, a FDA endorsed ‘Medication Guide’ or flier from the manufacturer. There is no ‘right way’, feel free to construct your own learning path.
Single Medication Patient Decision Aids:
Adaptable tools to compare 2 options
Long Format Patient Decision Aids
Our long format Patient Decision Aids were the first tools we developed, in 2009, to structure a discussion comparing a ‘leading option’ to alternatives. It gives the decision maker a path to gather information, identify what is most important, move towards a decision, and reflect on their intentions. A good decision is informed, consistent with patient values and acted on.
To select the essential content for the PtDA, we conducted a needs assessment to identify the information patients needed to be ready to participate in selecting a new disease modifying drug. The study included a Delphi analysis to establish a consensus amongst a group of content experts of these core domains. Then we conducted a community-based survey of 628 RA patients randomly sampled from > 7000 RA patients seen in practices in 5 economically and ethnically diverse Michigan cities (Saginaw, Flint, Lansing, Kalamazoo and Grand Rapids). This was funded by a $250,000 MSU Innovation Grant. The details and findings can be found in the publication linked below.
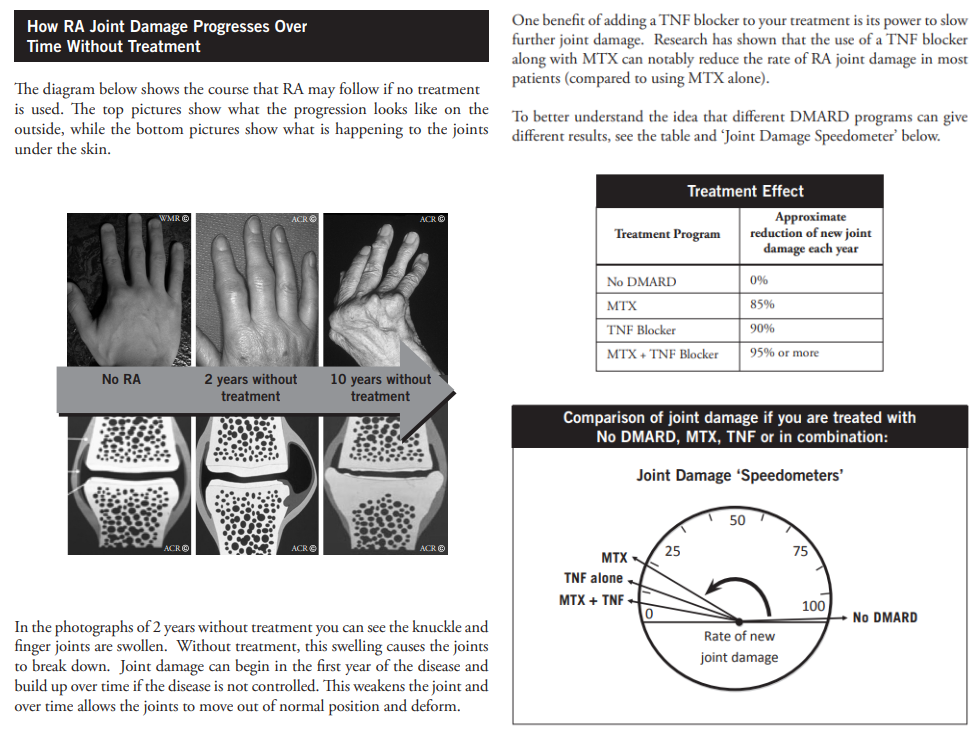
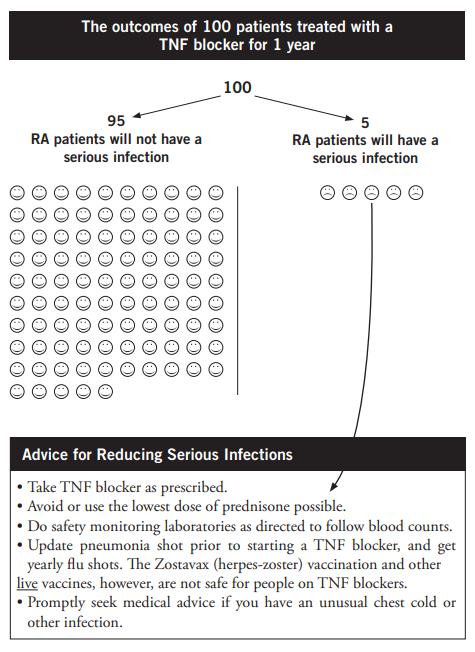
The next series of studies evaluated ways to present information about disease modifying medications and how patient characteristics influenced its reception. We evaluated important elements of information presentation for balance and bias. The gallery below shows some of the formats we found helpful in informing patients about disease modifying drugs (DMARD) potential benefits and harms.
Citations of our work
Martin RW, Raykov T, Head AJ, Feichtner J, Holmes-Rovner M. Rheumatoid Arthritis DMARD Knowledge Profile: Development and Validation. Arthritis Rheum 2006;54:S700.
Martin RW, Swartz T , McIntyre B, Holmes-Rovner M. Effectiveness of Disease Modifying Anti-rheumatic Drug Risk Communication in Rheumatoid Arthritis. Arthritis Rheum 2006;54:S369.
Martin RW, Bader LA Head AJ Turbergen EJ, Holmes-Rovner M. Identifying Patients Who Need Low Literacy Materials to Support Anti-Rheumatic Drug Decision Making. Arthritis Rheum 2007;56:S109.
Martin RW, Holmes-Rovner M, Raykov T. Does Depression Modify Patient Appraisal of Anti-rheumatic Drug Treatment Effects? Society for Medical Decision Making Pittsburg, PA 2007.
Martin RW, Head AJ, Holmes-Rovner M. Ability to Interpret Statements of Numeric Risk and Patient Satisfaction with Anti-Rheumatic Risk Communication. Society for Medical Decision Making Pittsburg, PA 2007.
Martin RW, Gallagher PJ, Eggebeen AT, Head AJ. A Decision Aid for Rheumatoid Arthritis Patients Considering Methotrexate Therapy. Arthritis Rheum 2009;60:S324.
Martin RW, Gallagher PJ, Tellinghuisen DJ. Can the Results of Laboratory Based Message Framing Experiments Be Generalized to Patients? Plenary presentation Society for Medical Decision Making. Chicago, IL. 2011.
Martin RW, Head AJ., Birmingham JD, Eggebeen AT. Does Biased Risk Perception Explain the Underuse of Disease Modifying Anti-Rheumatic Drugs? Arthritis Rheum 2012;64 Suppl 10 :382 DOI: 10.1002/art.38117.
Nallani R, Martin RW. Decisional Conflict in Doctor – Patient Discussions about Disease Modifying Anti-Rheumatic Drugs [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/decisional-conflict-in-doctor-patient-discussions-about-disease-modifying-anti-rheumatic-drugs/.
Bruce EJ, Martin RW. Impact of known versus unknown information about biologic therapy on motherhood choices in inflammatory arthritis. Poster presentation. Society for Medical Decision Making Oct 2021. Manuscript in review.
Short Format Patient Decision Aids
Our short format Patient Decision Aids are an quick tool to structure a discussion comparing a ‘leading option’ to alternatives. It then gives the decision maker structure to move towards a decision, identify what is most important and then reflect on the decision made.

Finally, we compared the long 24-page and short 2-page format with a FDA endorsed pharmaceutical industry information booklet in a randomized controlled study in biologic naïve RA patients considering taking etanercept (Enbrel). Read the supporting publication from the scholarly journal ‘Medical Decision Making’ to learn the surprising lessons. Hint: Beliefs about potential benefit and social norms, possibly mediated by evaluative conditioning, were more important than knowledge or beliefs about possible medication harms in molding perception of risk and medication choice.
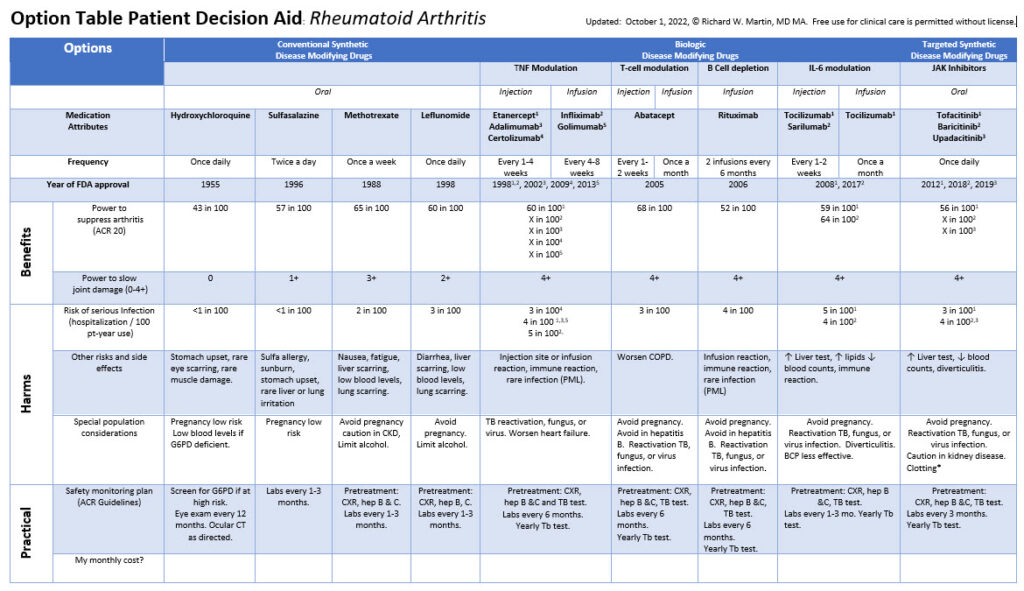
Option Table Decision Aids:
Tools to Structure and Support Physician Patient Dialogues About High Stakes Medications
Option Table Patient Decision Aids summarize and compare the features of disease modifying anti-rheumatic drugs (DMARD). They source facts from the FDA Prescribing Information (estimating point estimates of outcomes using meta-analytic methods) and then confirm or expand on gaps in the picture from trusted sources like the Cochrane Reviews or other peer reviewed meta-analyses. To be transparent, the back side of each PtDA lists each of these sources.
In our first phase of this concept, we developed decision aids for three separate choice sets: selecting your 1st DMARD, selecting your 2nd DMARD and selecting your 3rd or later DMARD. Patients (and physicians) loved this ‘swimming lane’ approach. It met our goal of a simple ‘job aid’ that physicians could annotate and reduce until in dialogue patient priorities surfaced.
Next, we moved towards efforts to disseminate the use of patient decision aids by partnering with colleagues at Forefront Collaborative, an innovative multiplatform CME program developer. This has led to a number of face to face as well as online interventions teaching shared decision-making using patient decision aids to rheumatologists dermatologists, physician assistants and nurse practitioners. Several thousand providers have participated. Pre-COVID venues have included the American College of Rheumatology National Scientific Meeting, Maui Dermatology and related mid-level provider focused conferences in Ashville, NC, Scottsdale, AZ and Las Vegas, NV.
Read a case study of a program conducted in association with the 2018 American College of Rheumatology Scientific Meeting. https://forefrontcollab.com/case-studies/chat-rheum/
Reported at the American College of Rheumatology 2020 National Scientific Meeting

During COVID we focused on online CME interventions to teach clinicians how to apply shared decision-making skills when applying clinical practice guidelines addressing COVID-19 infection and vaccination that are relevant to patients with Psoriatic Arthritis. We developed self-directed experiences, which incorporated patient perspectives, of building and solving patient cases to learn from making decisions and receiving immediate feedback. Activities included a skill-oriented presentation on engaging patients in shared decision making, decision aids, and a demonstration of an augmented reality (AR) app on PsA for healthcare providers and patients. You can download the ImmerseRx: Psoriatic Arthritis augmented reality app on your mobile device.
Rheumatoid Arthritis
In our next iteration we developed a more concise format that printed all FDA approved DMARD attributes on two sides of legal paper. This included a open space as a prompt a discussion to estimate what out of pocket costs might be.
Psoriatic Arthritis
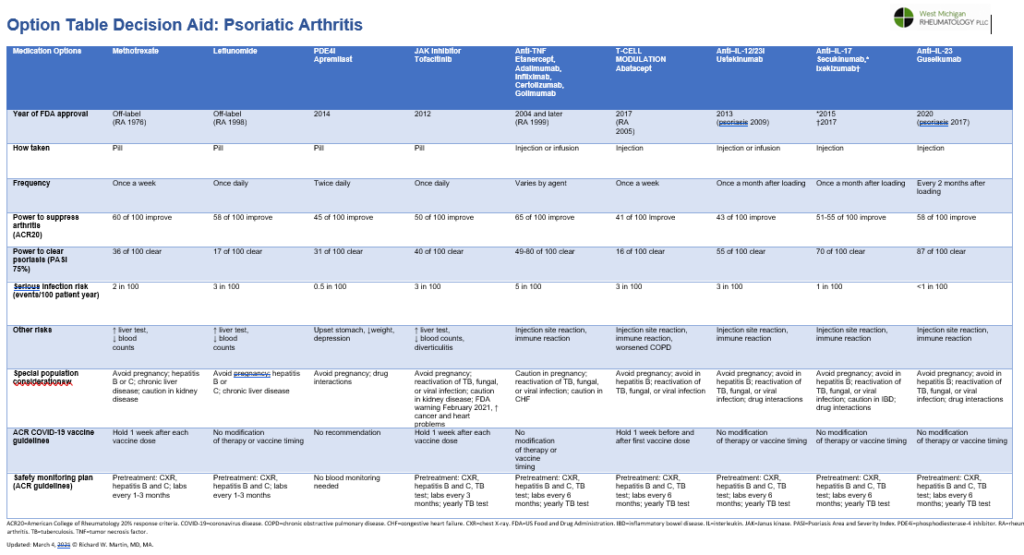
The design of a decision aid for psoriatic arthritis is a bit more complicated as there are two disease phenotypes: peripheral arthritis and axial disease. Each has its own medically reasonable choice set. We have have medications that regulate psoriatic arthritis through a variety of pathways.
In each case there is an important trade off of the power to suppress arthritis, clear psoriasis and risk of serious infection. This option table helps to cut through the clutter of information and focus on the details that are important in your decision.
Explore a CME Learning Activity that integrates SDM and PtDAs
We have a partnership with Forefront Collaborative and colleagues at the University of Wisconsin to develop online training activities for rheumatology clinicians (MD, DO, PA, NP) to improve there skills using Shared Decision Making to communicate with patients about new treatments for rheumatoid arthritis and psoriatic arthritis. Click the links below to take part in one of these free educational programs.
Turning Talk Into Treatment
Despite advances in treatment, navigating the rapidly evolving therapeutic landscape of psoriatic arthritis (PsA) can be challenging for both clinicians and their patients. Turning Talk Into Treatment is designed to help bridge the gap between available treatment options and patient care to enable clinicians to find a clear way forward.
In this free one-hour activity, two rheumatology faculty members will share the latest treatment recommendations from the ACR and GRAPPA. They’ll also explain the how you can use shared decision making with your patients to help them consider new treatment options.
Building the Case for Change
Despite treatment advances, many people living with rheumatoid arthritis (RA) don’t have their disease adequately controlled. In this activity, you’ll learn about the evolving therapeutic landscape in RA treatment, including updated clinical practice guidelines and the latest evidence for the efficacy and safety of Janus kinase (JAK) inhibitors.
After that, you’ll apply what you’ve learned about RA treatment guidelines and options through interactive, personalized case studies. You’ll build your cases by choosing patient characteristics, the disease activity, and a comorbidity or special circumstance. Each case will lead you through making a clinical decision and receiving expert feedback about your decision.
Shared decision making between patients and providers encourages patients to effectively use self-management strategies which can improve treatment adherence and satisfaction. In this 45-minute activity, you’ll learn about the steps that make up the shared decision making process, and watch a rheumatologist and a patient with RA engage in the shared decision making conversation.